Embryonic stem cells used to regrow nerve connections in patients with spinal cord injuries
Preliminary results have recently been presented on a early-phase clinical trial that aims to treat paralysis as a result of spinal cord injury. Embryonic stem cells differentiated into early nerve cells are used to repair injury to nerves in the spinal cord. The researchers hope to restore muscle function in these recently paralyzed patients. Other phase I/II trials using neural and mesenchymal stem cells to date are near completion, but this study is the first to use stem cells of embryonic origin.
A full report including follow-up of the included patients is expected in January 2017, but a presentation at the meeting of the International Spinal Cord Society in September 2016 showed positive early results1. Five patients with a high spinal cord injury have received the treatment and have improved, albeit still limited, function of the arms and hands compared to the starting point. The project is supported by Asterias Biotherapeutics and is a phase 1/2a study, designed as an open label trial with a single study arm. Increasing doses of cells will be administered to different groups over the course of the study.
Dr. Fessler, neurosurgeon at Rush University Medical center says this treatment may bring a change after many futile attempts to recover paralyzed patients. Dr. Fessler is quoted saying “Until now, there have been no new treatment options for the 17,000 new spinal cord injuries that happen each year. We may be on the verge of making a major breakthrough after decades of attempts.”2
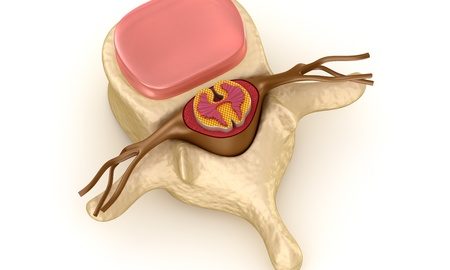
Spinal cord injury results in paralysis through the disruption of neural circuits between the brain and the target organ/limb. An interruption causes partial or complete loss of sensation, muscle function and the autonomic functions that keep our body in balance. Depending of the level of the injury, the paralysis can occur in both the arms and legs (quadriplegia, in lesions of the neck) or just the legs and torso (paraplegia, in lesions below the neck). Physical traumas, specifically from motor vehicle accidents, to the neck or back are the most common cause of spinal cord injury. Other causes include degeneration of the spine, which protect the spinal cord, resulting from old age or cancerous tumors in the back. However, most injuries occur in males under 30 years of age. Which means a lifetime of limited mobility.
In this multicenter study 10 million stem cells are injected into the site of injury 2 and 4 weeks after the injury. Embryonic stem cells are converted into AST-OPC1 (oligodendrocyte progenitor cells). Oligodendrocytes are supportive cells in the brain and spinal cord. They form the protective (myelin) sheath around neural axons (fibres). The theory is that injecting these cells will support regeneration of new networks at the site of a spinal cord injury.
The study is still including new patients between 18 and 65 years old with a recent spinal cord injury to the neck, which has resulted in paralysis of arms, torso and legs. Inclusion of sufficient patients will help demonstrate the effect of this treatment, which offers new hope after many years of stagnated development in the management of such injuries. This early clinical study aims to show safety and efficacy of the tested doses. It is important to note that future studies will need to include a control group to demonstrate superiority over a placebo treatment.
The presentation by Edward Wirth, chief medical officer of Asterias, from September 14th can be found in the first link below.
Resources:
- http://asteriasbiotherapeutics.com/wp-content/uploads/2016/09/Wirth-ISCoS-14SEP2016-talk-FINAL.pdf
- http://www.bionews.org.uk/page_701647.asp


