Is The Cure For Osteoporosis Coming Soon?
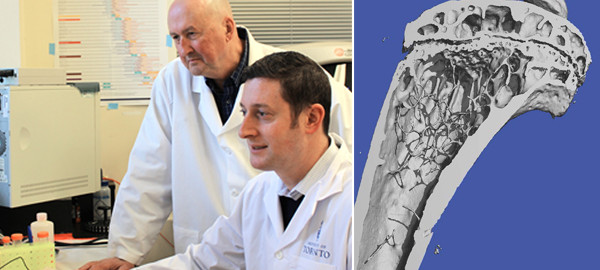
Mesenchymal Stromal Cell Transplantation Prevents Functional Bone Loss in a Mouse Model of Age-Related Osteoporosis
Osteoporosis presents significant morbidity and healthcare burdens. It affects over 200 million people worldwide. Osteoporosis can be a life threatening condition in the elderly. Age-related osteoporosis is a bone formation dysfunction which results from defective proliferation and differentiation of mesenchymal stem cells (MSCs). This leads to damaged bones, loss of bone volume, loss of microarchitectural integrity as well as inability to perform remodeling-mediated maintenance of the skeleton by MSCs. A study showed that MSCs obtained from osteoporotic mice show increased apoptosis in culture, and the reduced proliferative ability was coupled to increased apoptosis in MSCs from osteopenic mice[1].
MSCs are multipotent stem cells capable of self-renewal. MSCs reside in the stroma of bone marrow and can differentiate to form different lineages such as adipocytes, cartilage, bone, tendons, muscle, and skin. Owing to their self-renewal properties, these cells have enormous therapeutic potential in regenerative medicine for tissue repair. MSCs were first identified more than four decades ago in a pioneering study by Friedenstein and Petrakova [2]. The term “mesenchymal stem cell” was coined in 1991 by Arnold Caplan [3]. More than 500 clinical trials with MSCs have been reported to date (http://www.clinicaltrials.gov) including treatment of some bone related conditions.
A research group led by Dr. William Stanford in Ottawa, Ontario anticipated that if defective MSCs are responsible for osteoporosis, then transplantation of healthy MSCs should be able to prevent or treat osteoporosis. To test this possibility, they isolated MSCs from the bone marrow of 5-6 month old wild type mice and harvested the MSCs at low passage. 2X106 MSCs cells were injected via tail vein into a Sca1-/- mouse model of human age-related osteoporosis[4]. Sca1-/- mice undergo normal bone development, but with age, exhibit dramatically decreased bone mass resulting in brittle bones. Sca1-/- mice exhibit deficiency in MSCs to support bone formation which leads progressive bone loss and mechanical weakness beyond age 6 months. These mice serve as a good model for human type II osteoporosis[5] with a low-turnover state, old, hyper mineralized and mechanically inferior bone.
It was observed in this study that donor MSCs were capable of residing in the recipient mice bone marrow after 2 weeks of transplantation. Moreover, MSCs from donor were capable of long term engraftment.
The injected Sca1-/- mice showed increased bone formation, bone quality and sustained microarchitectural competence after 24 weeks of transplantation with just a single dose of MSCs. The transplanted mice displayed normal trabecular connectivity and anisotropy.
This phenomenal study establishes proof that MSC transplantation may be a viable therapeutic strategy to treat or prevent human age-related osteoporosis. As a next step in this direction, Dr. Jeff Kiernan, the first author of this study, says, “We’re currently conducting ancillary trials with a research group in the U.S., where elderly patients have been injected with MSCs to study various outcomes. We’ll be able to look at those blood samples for biological markers of bone growth and bone reabsorption.”
If improvements to bone health are observed in these ancillary trials, according to Professor Stanford, larger dedicated trials could follow within the next five years.
References:
[1] G. Turgeman, Y. Zilberman, S. Zhou, P. Kelly, I. K. Moutsatsos, Y. P. Kharode, L. E. Borella, F. J. Bex, B. S. Komm, P. V. N. Bodine, and D. Gazit, “Systemically administered rhBMP-2 promotes MSC activity and reverses bone and cartilage loss in osteopenic mice.,” J. Cell. Biochem., vol. 86, no. 3, pp. 461–74, Jan. 2002.
[2] A. J. Friedenstein, I. I. Piatetzky-Shapiro, and K. V Petrakova, “Osteogenesis in transplants of bone marrow cells.,” J. Embryol. Exp. Morphol., vol. 16, no. 3, pp. 381–90, Dec. 1966.
[3] A. I. Caplan, “Mesenchymal stem cells.,” J. Orthop. Res., vol. 9, no. 5, pp. 641–50, Sep. 1991.
[4] J. Kiernan, S. Hu, M. D. Grynpas, J. E. Davies, and W. L. Stanford, “Systemic Mesenchymal Stromal Cell Transplantation Prevents Functional Bone Loss in a Mouse Model of Age-Related Osteoporosis.,” Stem Cells Transl. Med., Mar. 2016.
[5] M. Bonyadi, S. D. Waldman, D. Liu, J. E. Aubin, M. D. Grynpas, and W. L. Stanford, “Mesenchymal progenitor self-renewal deficiency leads to age-dependent osteoporosis in Sca-1/Ly-6A null mice.,” Proc. Natl. Acad. Sci. U. S. A., vol. 100, no. 10, pp. 5840–5, May 2003.
Image courtesy of http://news.engineering.utoronto.ca/


